I’ve never thought of myself as particularly obedient, especially when it comes to health advice delivered in bullet points and cheerful fonts. But when it comes to vaccines, I don’t hesitate. I get every single one I can. Flu. Shingles. Covid. RSV. If there’s a sleeve to roll up, mine is already halfway there.
Part of that is practical. I travel not aspirationally, not someday, but actually. Airports, trains, long days on my feet, recycled air, unfamiliar bugs. Travel exposes you to the world in all its beauty and all its bacteria, and I’m not interested in sacrificing weeks or months of hard-won mobility to something preventable.
There are also people who are firmly anti-vaccine. This essay isn’t for them. They won’t appreciate it, and that’s fine. I’m not trying to convert anyone. I’m writing for people like me, mature travellers who still want to move through the world with curiosity and clarity, who plan trips years ahead, and who understand that freedom often depends on reducing avoidable risks.
But the deeper reason is personal.
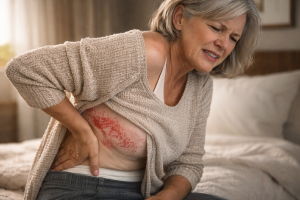 My Mum got shingles. It wasn’t a footnote in her life; it took over. The pain was relentless, exhausting, and far more severe than people tend to imagine when they hear the word. It lingered. It changed how she slept, how she moved, how she showed up in her own days.
My Mum got shingles. It wasn’t a footnote in her life; it took over. The pain was relentless, exhausting, and far more severe than people tend to imagine when they hear the word. It lingered. It changed how she slept, how she moved, how she showed up in her own days.
A dear friend of ours went through it, too, and it was awful. He had shingles so severely that clothing became unbearable. Fabric against skin was agony. He ended up nude at home and eventually went to a nudist beach simply because it was the only place his body could tolerate being. That detail may sound extreme, but it’s true. I should mention that he did like going to nude beaches. But it tells you everything you need to know about how dismissive we are of this illness until it lands in our own lives.
Those experiences rewired how I think about prevention.
What’s changed more recently and what surprised me is learning that vaccines may be doing far more than we once thought. They’re not just preventing specific infections; they appear to reduce a cascade of downstream problems that quietly derail aging: hospitalizations, cardiovascular events, prolonged inflammation, even cognitive decline.
Researchers call these “off-target benefits.” I think of them as quiet protection.
Flu vaccines, for example, are associated with lower risks of heart attacks, strokes, and heart-failure hospitalizations in older adults. Shingles vaccination has been linked, across multiple large studies, to lower rates of dementia later in life. RSV vaccines dramatically reduce hospitalizations from a respiratory virus that can be devastating as we age. Covid vaccination lowers the risk of long Covid, which anyone dealing with lingering fatigue or brain fog will tell you is no small thing.
These findings aren’t framed as guarantees — and they shouldn’t be. Most of this research is observational. Scientists are careful to say association, not cause. People who choose vaccination may also make other health-protective choices. Researchers adjust for age, sex, education, and chronic illness, but nuance remains.
What’s different now is scale.

These patterns are being identified across tens of millions of people, across continents, using modern statistical methods — and increasingly, AI-assisted analysis to synthesize enormous bodies of research that would once have taken decades to connect. That doesn’t make the findings magical. It makes them harder to ignore.
For travellers, the implications are very real. Hospital stays are brutal when you’re older, especially away from home. They disrupt routines, sleep and confidence. Delirium and deconditioning are common, and recovery often takes longer than anyone expects. Anything that lowers the chance of landing in a hospital bed also lowers the chance of coming home changed in ways you didn’t plan for.
I also want to be clear about respect. Not everyone can be vaccinated easily. Some people have compromised immune systems, autoimmune conditions, allergies, or medical histories that make these decisions complex or risky. Those realities deserve compassion, not judgment. Preventive care is never one-size-fits-all, and anyone navigating that terrain thoughtfully is already doing serious work.
For me, vaccines are part of travel planning. Right alongside good shoes, decent insurance, pacing myself properly, and knowing when to rest. They’re not about fear or virtue. They’re about continuity. About protecting memory, mobility, and the ability to say yes to the next trip instead of explaining why it had to be cancelled.
So yes, I get every shot I can. Not because I expect perfection, but because I want fewer interruptions. Fewer detours. Fewer stories that begin with “we never made it.”
At this stage of life, that feels less like compliance — and more like strategy.
Resources & Research Links
Shingles (Herpes Zoster) — CDC
https://www.cdc.gov/vaccines/vpd/shingles/public/index.html
RSV Vaccine Information for Older Adults — CDC
https://www.cdc.gov/rsv/clinical/index.html
Flu Vaccination & Prevention — CDC
https://www.cdc.gov/flu/prevent/vaccinations.htm
Pneumococcal Vaccine for Adults 50+ — CDC
https://www.cdc.gov/vaccines/vpd/pneumo/index.html
Meta-Analysis: Vaccination and Reduced Dementia Risk — Age and Ageing
https://academic.oup.com/ageing/article/51/8/afad125/6988026
Influenza Vaccination and Cardiovascular Risk — New England Journal of Medicine
https://www.nejm.org/doi/full/10.1056/NEJMoa043911
COVID-19 Vaccination and Long COVID — CDC
https://www.cdc.gov/coronavirus/2019-ncov/long-term-effects/index.html
Note: Statistical insights referenced above are drawn from peer-reviewed research and synthesized using modern AI-assisted literature analysis tools to identify consistent patterns across large populations.



